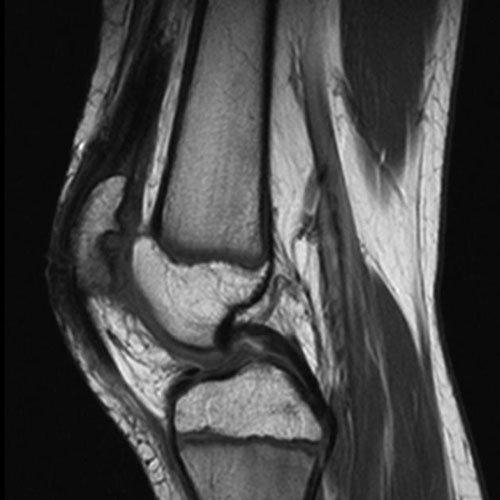
Chondromalacia patellae

X-Ray showing patellar malalignment
It is a painful condition of the knee which arises due to softening or wear and tear of kneecap cartilage. Cartilage under the kneecap acts as a shock absorber. Overuse, injury and many other things can cause deterioration of the quality and breakdown of the cartilage. Kneecap cartilage no longer remains smooth and agile and produces pain while coming in contact with thigh bone during different activities. Symptomatic presentation of chondromalacia patellae is very much similar to patellofemoral pain syndrome. But chondromalacia patellae is associated with cartilage damage whereas patellofemoral pain syndrome is not.
It affects young adults especially females more than any other age group. Common among runner, jogger, skier, soccer player, tennis player, cyclist, industrial and other professionals who need to kneel and squat for long hours or require repeated stairs and slope negotiation. Exact aetiology of chondromalacia patellae is poorly understood. During knee movement the knee cap glides smoothly over the groove of the thigh bone. Which is ensured by the balancing act of different stabilizing factors like thigh muscle, patellar tendon, ligaments, limb alignment and relative contour between knee cap and thigh bone groove.
Any deviation of these can cause rubbing or grinding of knee cap over thigh bone groove instead of gliding. Abnormal rubbing and grinding of the knee cap causes damage to its cartilage and development of chondromalacia patellae. Following factors can hamper smooth gliding of knee cap over thigh bone:
- Increase femoral anteversion; intoeing gait
- Excess valgus of knee; abnormal Q-angle
- Dynamic valgus of knee
- Pronation of foot
- Tight leg muscle; hamstring, iliotibial band, gastrocnemius
- Weak thigh muscle; quadriceps
- Imbalance between medial and lateral structures of knee cap; tight lateral retinaculum,
- weak vastus medialis (medial fibres of quadriceps muscle)
- Abnormal position of knee cap; patella Alta / patella Baja
- Abnormal relative contour of patellofemoral joint; trochlear dysplasia
Most common symptom is dull aching pain at the front of the knee underneath the kneecap during squatting, getting up from sitting position, going up and down stairs, going uphill and downhill. While asking to identify the location of pain patients cover the entire front of the knee. This can aggravate stiffness after prolonged sitting like watching a movie in theatre, travelling long in a car or plane. Sometimes the knee can get swell-up with accumulation of knee fluid. A cracking sound or grinding sensation can be felt while moving the knee joint. However, having this does not always mean chondromalacia patellae. On examination patellofemoral tenderness is very much evident and can be evoked by different manoeuvres.
Knee x-ray in three plane A/P, lateral and skyline view is the standard basic requirement. In the early case x-ray is non-conclusive. It can detect secondary bony changes in advance. Skyline view plays a key role to assess patellofemoral joint alignment. Only MRI can diagnose early cases of chondromalacia patellae. MRI and arthroscopy are the gold standard for diagnosis and assess the severity of cartilage changes in chondromalacia patellae which is described by grading. MRI is non-invasive whereas arthroscopy is invasive and logistically unacceptable only for diagnosis purposes.
- Grade I: Only softening of knee cap cartilage. MRI shows signal changes only
- Grade II: Softening along with shredding of cartilage surface. MRI shows signal changes along with disruption of cartilage integrity.
- Grade III: Thinning of knee cap cartilage. MRI shows thinning of cartilage with signal changes in bone.
- Grade IV: Total shredding off the cartilage exposing the underlying bone which can also be detected on MRI.
Treatment of Chondromalacia patellae is difficult as no single mode of treatment is a full proof method to ensure desirable outcome. Physical therapy is the mainstay of the treatment regime. It helps symptom relief by offloading the knee cap by improving knee muscle strength and gait. Analgesic and icing is helpful in acute conditions and recommended for short duration. Commonly practised medical and semi-interventional treatments are,
- Chondroprotective dietary supplement like glucosamine and chondroitin
- Intra articular injection of hyaluronic acid
- Intra-articular injection of PRP (platelet rich plasma)
All of these are being practiced widely with good results. But the outcome is not uniform and sometimes unpredictable. These treatments are effective in the early stage of disease only. Surgical treatments are indicated in advance stage of disease and for non-responder to medical management. Different surgical treatments are recommended and practised,
- Arthroscopic debridement of damaged cartilage and marrow stimulation (Microfracture)
- Arthroscopic release of plica and tight lateral structures
- Patellar realignment surgery